Duchenne muscular dystrophy (DMD) is a recessive X-linked form of muscular dystrophy, affecting around 1 in 3,600 boys, which results in muscle degeneration and eventual death.
The disorder is caused by a mutation in the dystrophin gene, the largest gene located on the human X chromosome, which codes for the protein dystrophin, an important structural component within muscle tissue that provides structural stability to the dystroglycan complex (DGC) of the cell membrane.
While both sexes can carry the mutation, females rarely exhibit signs of the disease.
Symptoms usually appear in male children before age 6 and may be visible in early infancy.
Even though symptoms do not appear until early infancy, laboratory testing can identify children who carry the active mutation at birth. Progressive proximal muscle weakness of the legs and pelvis associated with a loss of muscle mass is observed first. Eventually this weakness spreads to the arms, neck, and other areas.
Early signs may include pseudohypertrophy (enlargement of calf and deltoid muscles), low endurance, and difficulties in standing unaided or inability to ascend staircases. As the condition progresses, muscle tissue experiences wasting and is eventually replaced by fat and fibrotic tissue (fibrosis). By age 10, braces may be required to aid in walking but most patients are wheelchair dependent by age 12. Later symptoms may include abnormal bone development that lead to skeletal deformities, including curvature of the spine. Due to progressive deterioration of muscle, loss of movement occurs, eventually leading to paralysis. Intellectual impairment may or may not be present but if present, does not progressively worsen as the child ages. The average life expectancy for patients afflicted with DMD is around 25.
Genetic testing may be useful for prospective parents who have a family history of MD and are worried about passing the condition on.Discuss with us for for genetic screening and counseling.
Genetic testing can be used to:
Genetic testing is likely to be used more often in the future, as knowing the precise cause of the MD may make a difference to what type of treatment will be most effective.
Some types of MD can be carried without causing clear signs of the condition. This applies to recessive inherited disorders, sex-linked conditions and even some dominant conditions. Genetic testing can determine who is carrying the disorder.
For example, a woman with a family history of DMD but no symptoms herself may be carrying the gene that causes it.
We need to identify the gene responsible for DMD in Family. It is best identified from the affected MALE member ( He could be her brother or her mothers brother!).
To be Mother can be evaluated for the possible genetic mutation from her blood and compared with a sample from a family member who has the condition to find out if she is carrying the faulty gene.
If you or your partner are a carrier of MD and are at risk of passing the condition on to your child, your genetic counsellor will discuss your options with you.
DNA test
The muscle-specific isoform of the dystrophin gene is composed of 79 exons, and DNA testing and analysis can usually identify the specific type of mutation of the exon or exons that are affected. DNA testing confirms the diagnosis in most cases
DMD is the disorder where a part of chromosome X is deleted. There is a possibility of deletion ( Defect) of different 79 types.As you know that female has 2 X chromosome and Male has ONLY one X chromosome. An X-linked recessive gene carries DMD.
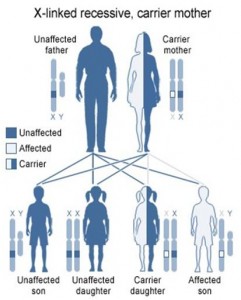
Males have only one X chromosome, so one copy of the mutated gene will cause DMD. Fathers cannot pass X-linked traits on to their sons, so the mother transmits the mutation.
If the mother is a carrier, and therefore one of her two X chromosomes has a DMD mutation, there is a 50% chance that a female child will inherit that mutation as one of her two X chromosomes, and be a carrier. There is a 50% chance that a male child will inherit that mutation as his one X chromosome, and therefore have DMD.
Prenatal tests can tell whether their unborn child has the most common mutations. There are many mutations responsible for DMD, and some have not been identified, so genetic testing only works when family members with DMD have a mutation that has been identified.
Prior to invasive testing, determination of the fetal sex is important ,which is officially permitted under PCPNDT Act in India, while males are affected by this X-linked disease, female DMD is extremely rare.
This can be achieved by ultrasound scan at 14 weeks or more recently by free fetal DNA testing. There are two main ways of performing prenatal diagnosis. One is chorionic villus sampling (CVS). This is when tissue from the placenta is removed for analysis, usually after no less than 11 weeks into the pregnancy. The other method is amniocentesis, which is not usually carried out until 16 weeks of pregnancy. In amniocentesis, a needle is inserted into uterus to take a sample of the amniotic fluid that surrounds the fetus in the womb. This fluid contains cells that have been shed by the fetus. Both of these tests carry a small risk of causing miscarriage.
The cells from the fetus can be tested to determine whether they have the genetic mutation responsible for DMD. If they do, the baby is likely to develop DMD at some stage after birth.
Another option in the case of unclear genetic test results is fetal muscle biopsy.
If this is the case, we will be able to discuss your options with you, which will often include terminating the pregnancy. Such decisions can be very difficult and very personal, and different people have very different feelings about what to do.
Be aware that there are limitations to this kind of diagnosis. Tests can give misleading or unexpected results. It is important to discuss prenatal testing and the meaning of the possible results before going ahead with the procedure.
